Ambriel vs Assured
Side-by-side comparison to help you choose the right tool.
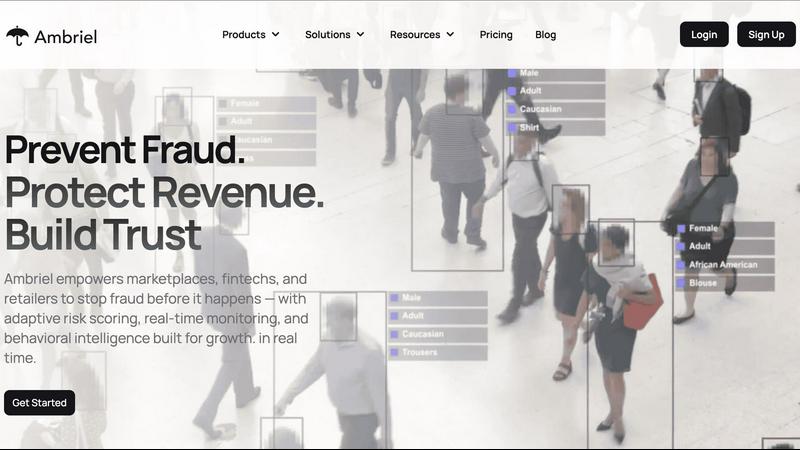
Ambriel enables businesses to detect and prevent fraud in real-time, protecting revenue and enhancing customer trust.
Last updated: March 1, 2026
Assured
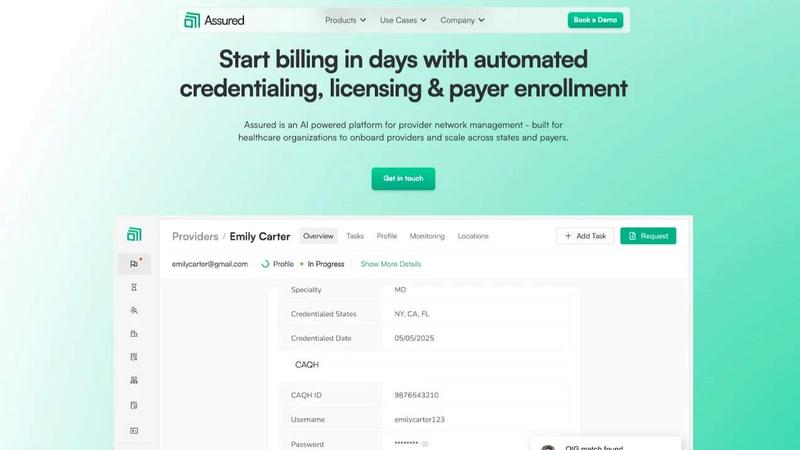
Assured uses AI to automate healthcare provider credentialing so you can start billing in days, not months.
Last updated: April 13, 2026
Visual Comparison
Ambriel
Assured
Feature Comparison
Ambriel
Advanced Fraud Detection
Ambriel employs AI-driven risk scoring, tapping into data from over 200 sources to spot suspicious activities in real time. This feature is crucial for protecting revenue before it succumbs to fraud, allowing businesses to act quickly and decisively.
Sanctions & PEP Screening
This feature automates compliance by screening against over 100 global sanctions, politically exposed persons (PEP), and crime lists. Manual checks become a thing of the past, simplifying the compliance process and enabling businesses to maintain a robust growth trajectory.
Continuous Monitoring
With 24/7 tracking of transactions and accounts, Ambriel provides alerts on unusual patterns. This continuous oversight helps businesses identify potential fraud before it escalates into costly incidents, ensuring peace of mind for organizations and their customers.
Seamless Onboarding
Ambriel streamlines customer onboarding flows with automated checks that validate the trustworthiness of customers and sellers. This feature eliminates the friction that often hampers the user experience, allowing businesses to welcome only reliable users into their ecosystems.
Assured
AI-Powered Primary Source Verification
Assured's AI engine performs real-time, parallel verification across a staggering network of over 2,000 primary sources—from state medical boards to sanction lists. This eliminates the sequential, weeks-long manual chase, delivering comprehensive credentialing packages in hours, not months, with unparalleled accuracy that slashes errors and audit risks.
Automated Payer Enrollment & Tracking
The platform automates the entire payer enrollment lifecycle. It intelligently generates payer-specific applications, submits them directly through portal integrations, and provides real-time tracking with automated follow-up reminders. This cuts through complex, unstable payer rules to get providers in-network 30% faster and achieve industry-leading first-pass approval rates.
Centralized Network Intelligence Hub
Assured consolidates all provider data—credentials, licenses, enrollments, and verifications—into a single source of truth. This centralized roster management supports all data formats and offers real-time monitoring dashboards, giving leaders complete visibility and ending the chaos of disconnected spreadsheets and outdated systems.
Proactive Licensing & Compliance Monitoring
Go beyond simple tracking. Assured proactively manages multi-state licensure and renewals across all 50 states, automating application submissions and sending alerts for expirations. Its continuous monitoring detects sanctions and compliance issues an average of 22 days earlier than manual methods, ensuring network integrity.
Use Cases
Ambriel
Onboarding & Registration Fraud
Ambriel effectively detects fake accounts, synthetic identities, and bot-driven signups at the registration stage. This proactive identification prevents fraudsters from exploiting platforms before they can infiltrate systems.
Payment & Transaction Fraud
Through real-time monitoring of transactions, Ambriel can pinpoint anomalies and prevent chargebacks. This vigilance helps to block fraudulent transfers, thereby safeguarding the financial health of businesses.
Bonus & Promotion Abuse
Ambriel is adept at identifying multi-accounting, referral scams, and the exploitation of incentive programs. By ensuring fair reward distribution, businesses can maintain the integrity of their promotional efforts.
Account Takeover Protection
This use case focuses on identifying unusual login behavior, device changes, and attempts at credential stuffing. By safeguarding accounts, Ambriel helps protect customers from unauthorized access and potential data breaches.
Assured
Rapid Scaling for Digital Health Startups
For digital health companies expanding into new states, manual credentialing is a growth killer. Assured automates state-by-state licensing and multi-payer enrollment from one platform, enabling startups to onboard providers in under a month and launch services in new markets without administrative delays or guesswork.
Health System Provider Network Optimization
Large health systems drowning in disparate systems use Assured to centralize network data and automate credentialing for hundreds of providers. The platform streamlines onboarding, ensures continuous compliance monitoring, and provides system-wide visibility, freeing up countless administrative hours and securing revenue.
Payer Network Expansion & Management
Health plans and payers leverage Assured to efficiently credential and onboard new providers into their networks at scale. The AI-driven verification and automated workflows ensure high-quality, compliant provider data, accelerating network growth and improving provider directory accuracy.
Multi-State Medical Group Expansion
Specialty provider groups, like dermatology or behavioral health practices, use Assured to manage the complex web of licensing and payer enrollments required for multi-state expansion. The platform handles state-specific nuances, allowing groups to credential specialists and get them seeing patients in weeks instead of months.
Overview
About Ambriel
Ambriel is an innovative fraud intelligence and risk management platform tailored for digital businesses striving for security and compliance. Its primary goal is to protect users and revenue while ensuring that legitimate activities remain uninterrupted. This makes Ambriel an indispensable tool for sectors such as fintech, online marketplaces, retail, and iGaming. By integrating behavioral analytics, device intelligence, sanctions screening, and real-time risk scoring, Ambriel creates a unified ecosystem that allows organizations to effectively identify, score, and prevent fraudulent activities. The platform analyzes a multitude of factors, including transactions, user behaviors, devices, and network signals, to reveal concealed risk patterns and automate mitigation processes. This proactive stance empowers businesses to combat various types of fraud—like multi-accounting, bonus abuse, referral fraud, synthetic identity creation, payment fraud, and money laundering—ensuring that both revenue and reputation are safeguarded.
About Assured
Assured is the AI-powered operating system for modern healthcare networks, engineered to dismantle the administrative bottlenecks that cripple growth and revenue. This isn't just another database; it's an intelligent automation platform that tackles the core, manual inefficiencies of provider network management. Built for forward-thinking provider groups, health systems, payers, and digital health companies scaling at speed, Assured transforms a traditionally 60+ day credentialing nightmare into a 48-hour streamlined process. Its core value proposition is stark: achieve 95% first-pass approval rates for payer enrollments, detect critical sanctions 22 days earlier, and stop losing thousands per provider to manual tasks. As an NCQA-certified CVO, Assured leverages parallel AI processing to verify credentials across 2,000+ primary sources simultaneously, auto-generate applications, and submit directly to payer portals. The result is a seismic shift from reactive, error-prone paperwork to proactive, data-driven control, enabling faster provider onboarding, accelerated revenue cycles, and complete compliance confidence—all centralized on a single, intelligent platform.
Frequently Asked Questions
Ambriel FAQ
What industries can benefit from using Ambriel?
Ambriel is designed to cater to various industries, including fintech, retail, e-commerce, iGaming, insurance, and crypto. Its versatile features adapt to the unique fraud challenges faced by each sector.
How does Ambriel ensure compliance with regulations?
Ambriel automates sanctions and PEP screening against extensive global lists, eliminating the need for manual checks. This capability helps businesses maintain compliance effortlessly while focusing on growth.
Can Ambriel integrate with existing systems?
Yes, Ambriel offers integrations with popular e-commerce platforms like Magento, Woocommerce, and Wix Commerce. This ensures a seamless implementation process that fits into existing workflows.
Is Ambriel suitable for small businesses as well?
Absolutely! Ambriel is built to accommodate businesses of all sizes. Its scalable solutions allow even small enterprises to leverage advanced fraud protection and risk management features without overwhelming their resources.
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing is a 60+ day manual process of sequential verifications. Assured's AI automates this, processing applications in parallel and integrating with 2,000+ sources to cut time to 48 hours. This efficiency saves organizations an estimated $4,200 to $5,800 in administrative costs per provider annually.
What makes Assured more reliable than manual processes or other vendors?
As an NCQA-certified CVO, Assured meets the highest industry standards for verification. Its AI-driven parallel processing eliminates human error and delay, delivering 95% first-pass approval rates for enrollments and detecting compliance issues 22 days earlier than manual tracking, ensuring unmatched accuracy and reliability.
Can Assured integrate with our existing systems like our ATS or EHR?
Yes. Assured features plug-and-play APIs designed for seamless integration with your existing tech stack, including Applicant Tracking Systems (ATS), Electronic Medical Records (EHR), and CRM platforms like Salesforce, ensuring data flows smoothly without manual entry or disruption to current workflows.
How does Assured handle ongoing compliance and network monitoring?
Assured provides continuous, real-time monitoring of your entire provider network. It automatically tracks license expirations, renewals, and scans for sanctions or adverse actions across primary sources, sending proactive alerts to prevent lapses and ensure your network remains fully compliant and audit-ready.
Alternatives
Ambriel Alternatives
Ambriel is a sophisticated fraud intelligence and risk management platform that empowers businesses to detect and prevent fraud in real-time, ensuring compliance and safeguarding revenue. By integrating advanced technologies, Ambriel addresses the unique challenges faced by digital enterprises in sectors like fintech, retail, and online marketplaces. Users often seek alternatives due to various reasons such as pricing, specific feature sets, or compatibility with existing platforms. When selecting an alternative, it's crucial to evaluate its fraud detection capabilities, compliance features, and the level of automation offered to ensure a seamless fit for your business needs.
Assured Alternatives
Assured is an AI-powered platform in the provider network management and credentialing space. It automates the complex, manual back-office processes for healthcare organizations, dramatically speeding up time-to-revenue. Users often explore alternatives for several key reasons. These can include budget constraints, the need for a different feature set, or specific platform requirements like deeper integration with existing practice management or EHR systems. The search is driven by the universal need to find the right operational fit. When evaluating options, focus on core capabilities. Look for solutions that offer robust automation, high accuracy rates, and direct payer integrations. Security certifications, like NCQA CVO status, and real-time monitoring for compliance are also critical differentiators in this high-stakes category.
